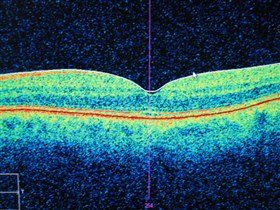
Optical Coherence Tomography (OCT) is one of the two major advances in ophthalmology over the past 10 years
The other is the discovery of Avastin (or Lucentis) – an injection into the eye that prevents the proliferation of destructive new blood vessels within the eye e.g. in macula degeneration or diabetic retinopathy
The OCT permits high resolution 2-D and 3-D views of the retina allowing all of the retinal layers to be easily identified. This makes the OCT an invaluable machine in identifying abnormality in these layers and makes the non invasive diagnosis of most retinal diseases much easier.
This patient presented after noticing small ring in the centre of their right eye vision. Using our regular examination techniques the eye looked normal
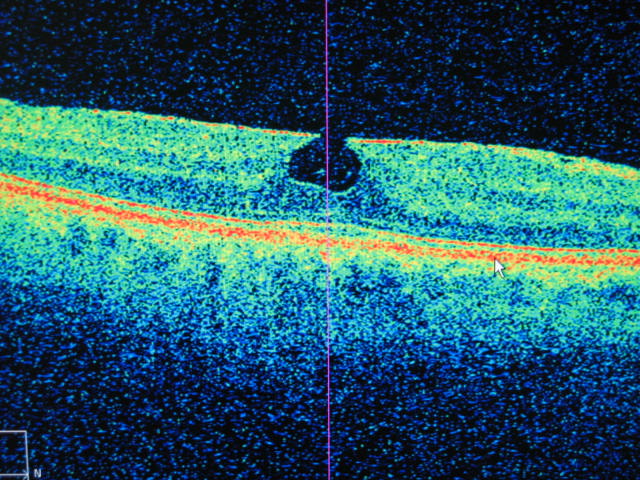
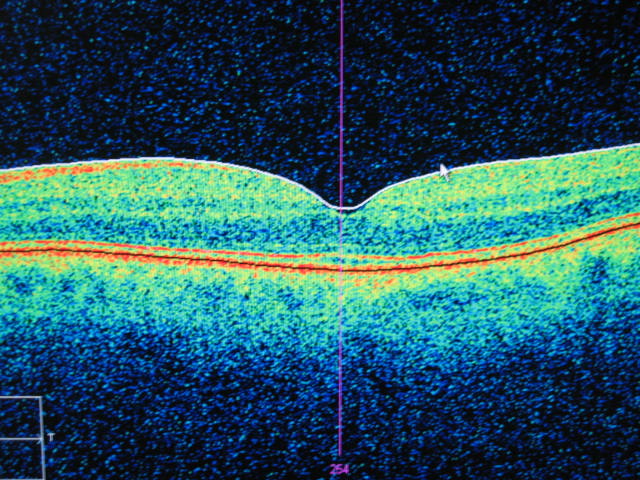
Only when we used the OCT could we see this abnormality – it shows all of the retinal layers but especially it shows a hole that shouldn’t be there (compare to the picture of the normal left eye below) (For the expert this is an obvious pseudo lamella hole at the macula caused by traction of a small epi-retinal membrane)
OCT also allows us to image and quantify the optic nerve head (ONH) and the retinal nerve fiber layer (RNFL) around the optic nerve head. Detected abnormality in the ONH or the RNFL can be the earliest sign of damage caused by glaucoma – but perhaps even more importantly – it can show more sensitively, change over time i.e. between visits
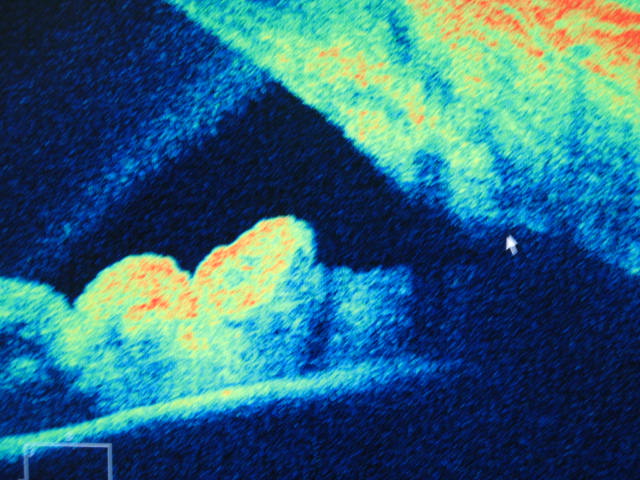
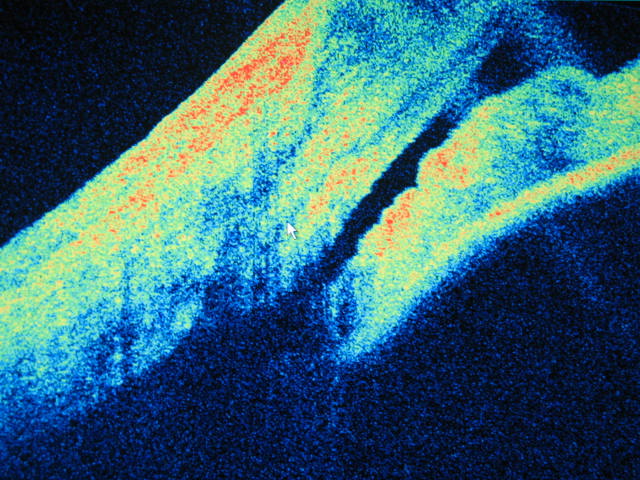
The cornea iris interface (the drainage angle of the eye) can also be imaged by OCT. This is relevant to the diagnosis of narrow angles that can lead to an acute form of glaucoma (sudden onset, very painful, red eye). Being able to identify these narrow angles before an acute angle closure attack means that preemptive (and simple) treatment to open the angle can be done by a medical eye specialist.
The first image below shows a wide open angle between the cornea and the iris and second shows a very narrow - but not closed angle
All our patients, here at McClellan Grimmer Optometrists will be offered an OCT exam when it is clinically indicated but especially where there is suspicion of glaucoma or where there is a strong family history of glaucoma, where there is unexplained central vision loss or where we need to further assess the macula or other retinal areas.

